Essential Tips for Managing a Meniscal Tear
A meniscal tear is a common knee injury that can cause pain, swelling, clicking, locking and limited movement in your knee. Proper management of a meniscal tear is crucial for a successful recovery whether this requires surgery or conserative management. In this blog post, we will provide you with essential tips to help you effectively manage a meniscal tear and aid in your rehabilitation process.
The meniscus is a piece of cartilage located in the knee joint. Each knee has two menisci, one on the inner side of the knee (medial meniscus) and one on the outer side (lateral meniscus). The menisci are C-shaped and act as shock absorbers and stabilizers for the knee. The primary function of the meniscus is shock absorption, joint stability and it provides a protective layer between cartilage surfaces.
How to manage a meniscal tear:
Consult a Medical Professional
The first step in managing a meniscal tear is to consult a medical professional. They will diagnose the severity of your injury and provide you with a personalized treatment plan. Send for an MRI if deemed clinical necessary and the earlier you start the process the better (Do not wait for it to settle down before seeing a physio!)
Rest, Ice, Compression, Elevation, MOVE
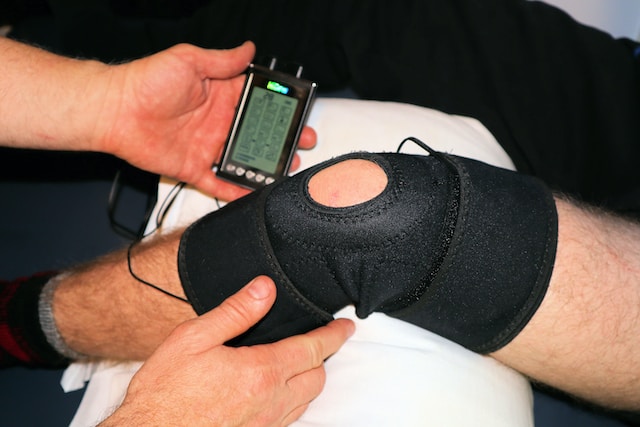
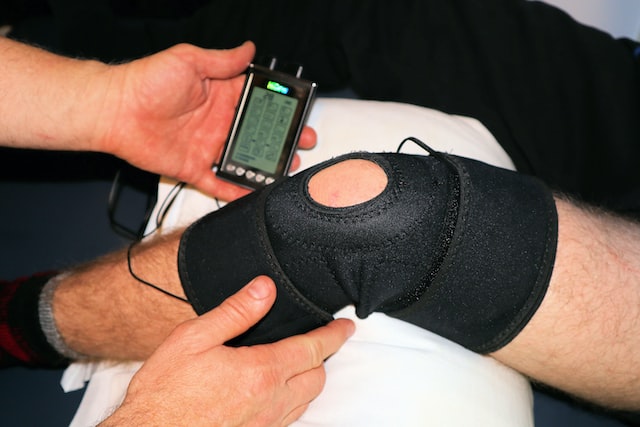
Start with this standard approach to manage many types of injuries. Rest your knee to avoid further damage, apply ice packs for 10-20 minutes every 2-3 hours to reduce swelling, use compression bandages to support the knee, and elevate your leg to minimize fluid accumulation. Start to gently move and activate the muscles surrounding the knee as soon as able.
Rehab Rehab Rehab
Rehabilitation is crucial for meniscal tear recovery. Your Physio will start gentle exercises targetting knee range of motion and quadricep strengthening. This can be progressed as tolerated for conservative management. If there is absence of locking, clicking and catching in the knee and sound conditioning program can restore the knee to normal function.
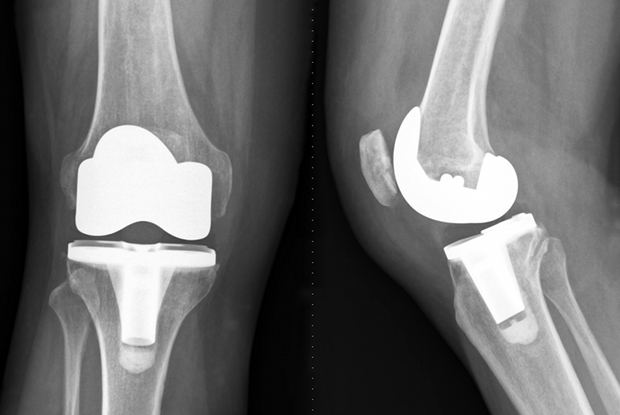
Surgery or No Surgery? You will need an MRI to help gauge the answer to this question.
- Surgical Intervention: In some cases, surgery may be necessary to repair or remove the torn meniscus. Arthroscopic surgery is a minimally invasive procedure commonly used for meniscal tear treatment. Your surgeon will determine the best course of action based on the tear’s location, size, knee symptoms, pain levels and activity limitations.
- Conservative Management: A good rehab program involving restoring good knee mechanics, restoring good strength of surrounding muscles and graded return to activity can be as good as surgery for a meniscus tear. BUT this depends on the levels of symptoms and how the knee tolerates exercise.
Graded return to sport and activities
As with any sport or activity. A graded return to sport and activity is very important and establishing good movement patterns prior to pushing the knee to hard. Prior to any running the knee should have good quads control, no swelling, minimal symptoms and your single leg squat and hop should be symmetrical to the non injured leg.
Managing a meniscal tear requires a comprehensive approach involving medical guidance, rehabilitation, and lifestyle adjustments. By following these essential tips, you can effectively manage your meniscal tear, promote healing, and restore optimal knee function. Remember, every individual’s condition is unique, so it’s crucial to consult your healthcare provider for personalized advice and treatment.
Reach out if you have had a recent knee injury.
Hit us up at info@thephysiodepot.com.au or Book Online Here